This month, my artwork I Will Wear My Heart Upon My Sleeve was published on the front page of The Intima: A Journal of Narrative Medicine! Check it out here:
Category Archives: Narrative Medicine Research
Autistic Strengths and Stereotypes, My First Publication
Two years after its conception, I have officially published a piece of my writing. After being lost in transition and undergoing a series of revisions, my review about literature for children with autism, Autistic Strengths and Stereotypes, has been published in Disability Studies Quarterly.
It’s been exciting for me to go through the publication process, to take an ordinary paper that I wrote for an independent study and turn it into something more. From corresponding with editors to revising and proofreading, I’ve enjoyed learning about the inner workings of the publication process. It’s an honor to be included as an author in one of my favorite journals.
Check it out! I’d love to hear your thoughts about my review:
Autistic Strengths and Stereotypes | Paul | Disability Studies Quarterly.
Sharing the Clinical Relevance of Narrative at the UM Pediatrics Research Symposium
Instead of numerical values and statistics, my poster shared the words and phrases of children with cancer. Amidst colorful posters with tables and graphs, my poster was adorned with drawings by pediatric oncology patients, such as cancer as a half-angel, half-devil being.
The 24th Annual Pediatric Research Symposium at the University of Michigan struck me as an interesting opportunity to share my narrative research with clinical pediatricians. I just began delving deeper into these narratives through a literary lens, and I enjoyed the challenge of reframing and furthering my analysis of these narratives for a medical audience. What does narrative illuminate about the living experience of childhood cancer? How do children conceptualize cancer and make sense of their illness experiences? And how can these narratives of pediatric oncology patients inform those who care for them?
Writing this abstract required more than inverting the active tense valued by the humanities to the passive tense valued in scientific writing. Designing this poster forced me to distill the numerous conversations and narratives that I have collected into a direct, concise argument. It was an incredibly helpful, albeit challenging, process.
From nearby poster presenters to practicing pediatric oncologists and more, it was interesting to discuss my research with a broad range of people and receive different feedback. One conversation in particular really resonated with me. A neighboring poster presenter asked me about my work, then confessed that she worked with pediatric oncology patients as a social worker for years. She said that it was a difficult and challenging position, one that ultimately surged her into depression because it was too much. To be able to work so intimately with these children, she said, “you need some kind of ‘distance.'”
This “distance” intrigues me. As we discussed this further, she explained that social workers preoccupy themselves primarily with the patients and families facing death, the ones struggling most with the interruptions of cancer. Physicians, on the other hand, have the chance to experience the broad range of paths that patients follow with cancer. The successful treatments, the ineffective drug regimens. This spectrum of outcomes helps give physicians perspective, but social workers by nature are honed in on the more despondent stories.
Is “distance” necessary for the emotional challenges of pediatric oncology? And if it is, what exactly does this imply about the impact of these childhood cancer narratives? I wonder, how might these narratives complicate and possibly challenge this notion of ‘distance’?
Contributing and Collaborating at the WMU Medical Humanities Conference
The people who I met, the conversations that we had, the ideas and passions that were exchanged and explored. These are the aspects that I enjoyed most at the Third Annual WMU Medical Humanities Conference, the things that I was most looking forward to and that I hope to experience at more conferences in the future.
I have to say, I think that this was one of my best presentations about my research. I’ve realized that I perform best as a speaker when I speak freely. The presentations that preceded mine throughout the day were inspiring. I felt my passion for my research empower me, and I was able to overcome anxiety with enthusiasm about my findings. The response to my presentation was overwhelmingly supportive and encouraging; some scholars were eager to share my project with students, others inviting me to stay in touch and explore their graduate programs. As the only student presenting, it was truly an honor to participate and I was fortunate to have such a great, interactive audience.
The entire conference was an adventure. From the woman who sat next to me on the shuttle bus to the Founding Dean of Western Michigan University’s Medical School, I had the opportunity to meet a variety of people. People had travelled from across the nation and as far as England to present and participate in this conference, to share the projects they were passionate about and to learn about the passions of others. With this interdisciplinary field, there was an interesting assortment of people: humanities and social science scholars, clinicians, educators, and many overlaps amongst these. Each presentation offered new insight about different facets of Medical Humanities, and the discussions that unravelled afterwards were equally engaging and thought-provoking. Being physically in the presence of Medical Humanities people helped me to better understand this field, and I’ll be incorporating some of my new thoughts from the conference in blog posts to come.
Here’s my WMU Medical Humanities Presentation: I wrote out notes in preparation, but they were by no means memorized. For those who would like to share my research with other students, I am honored. I really appreciate the support and enthusiasm!
Pondering Prepositions: Medical Humanities and Narrative Medicine
Rooted in the essence of humanity, health and medicine are inherently interdisciplinary. How are these fields intertwined with others? We express this entanglement through prepositions, mumbled words that can resound with significance.
Take, for example, literature. We can consider literature in/and/of medicine. There is a prepositional choice that we can make, one that urges us to consider the angle of our approach. We can do the same with other media forms like art.
In: Medical literature is present in medical education lectures, in research publications, in patient charts. Medicine has established an entirely different language with its own terminology, one that can manifest itself as a form of literature through scientific writing. The clinical practice of medicine is a dialogic exchange, a narrative. My understanding is that this area of study is largely encompassed by the field of Narrative Medicine, one that notes the literary merit of the medical practice.
Of: Literature has long been fascinated in the practice of medicine, its accomplishments and its qualms. There have been writings about medicine for centuries. Some are the stories of medical practitioners like William Carlos Williams, Oliver Sacks, Danielle Ofri. And others are written about the medical sphere from afar, such as the works of Ken Kesey, Elizabeth Moon, Sinclair Lewis. These literary texts seem to be the focus of Medical Humanities, which explores medicine through a literary lens.
And: I claim that this blog explores the intersection of literature and medicine: the ‘and.’ This intersection, however, is certainly a grey area. The ‘and’ balances the two fields, literature and medicine, declaring them as separate studies equal in merit. This introduces the idea that perhaps, because these are distinct, each has something to learn from the other. Maybe scholars can develop reading, writing, and critical thinking skills by confronting the medical profession through literature. Or analyzing literature can instill in health care professionals a different kind of care and compassion. The former feels more like Medical Humanities, the latter Narrative Medicine.
I believe that this is the realm shared by both Medical Humanities and Narrative Medicine. I’ve found that this grey area can be largely open to interpretation, but only through dissecting the fundamental threads within can we make sense of these fields and assemble these perspectives together.
Filed under Narrative Medicine Research
Illness Narratives, Medical Humanities, and Narrative Medicine
For the past few months, I’ve been on a mission to understand how illness narratives fit into the broader world of academia. I’ve encountered two primary schools of thought: Medical Humanities and Narrative Medicine. By talking to a variety of scholars in both fields, I’ve been trying to decipher how these fit together and what distinguishes them from one another. This is an introductory post to these concepts; throughout a series of posts to come, I hope to share some of my ideas about each of these fields, how they intersect, and where my own explorations of illness narratives may fall.
Medical Humanities is “an interdisciplinary field of humanities (literature, philosophy, ethics, history and religion), social science (anthropology, cultural studies, psychology, sociology), and the arts (literature, theater, film, and visual arts) and their application to medical education and practice.”
Narrative Medicine “fortifies clinical practice with the narrative competence to recognize, absorb, metabolize, interpret, and be moved by the stories of illness.”
Illness Narratives, as I define them, are “expressions about or around the experience of being ill.”
—
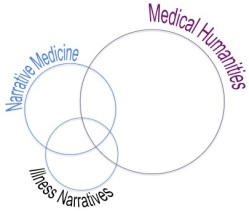
Loosely based on these definitions and largely based on my engagement with both fields, I’ve illustrated here my understanding of how these fields are related. There are overlaps, but there also exclusives. These evolving fields are not static but rather dynamic, shifting with the contributions of each individual.
What I’ve realized is that in the end, my study of illness narratives is not entrapped by these indefinite definitions. I can escape the boundaries of these words and instead find meaning in the margins. This isn’t an entirely satisfying conclusion, but I’m content with the realization that, for now, it is still in the works.
Filed under Narrative Medicine Research
Reconstructing the Past with ICU Patient Diaries
In permeating across disciplines, illness narrative research attains a level of potency, one that spans the globe. Dr. Ingrid Egerod, a nurse from the University of Copenhagen, spoke on Tuesday about “ICU patient diaries and follow up in Nordic countries.” She highlighted how narrative is being used by ICU nurses to enhance care in Nordic countries.
What is unique about ICU patients is that many spend weeks at a time unconscious, and later they are unable to remember the ICU. This dark vacuum of memory can be the cause of alarm for many patients, creating friction that sparks psychological discomfort for a patient in later years.
In the Nordic countries, nurses like Ingrid Egerod aim to fill this void by creating ICU patient diaries to capture the day-to-day lives of these patients. Unlike hospital charts, these records string together ICU events to create a coherent ICU experience. These diaries then become tools to aid patients in reconstructing their time in the ICU and creating their own illness narrative.
These have had an incredible impact on many members of the ICU scene, ranging from nurses to families to patients. This task seems to renew a sense of purpose for nurses and to help families to understand the progression of medical events through story. Egerod and others have demonstrated that patient diaries decrease the occurrence of Post-Traumatic Stress Disorder in ICU patients. After patients are presented with their diaries, nurses follow-up with them and use the diary as a guideline for conversation. These narrative activities are now being extended to include patients and families who are encouraged to use writing as a therapeutic form of expression.
It was fascinating to hear about this illness narrative research and to think about how narrative can adapt to and address the needs of the ICU unit and others. I also found it exciting to see that the idea of narrative is growing in other countries as well.
Here were some of the questions that I had, along with paraphrased answers provided by Dr. Egerod.
- How are these ideas being received globally?
There appears to be enthusiasm for narrative and a growing appreciation for the patient experience, but especially in countries like the U.S. where nurses are often overwhelmed as it is, the obligation of ICU patient diaries can become a burden. This is definitely an obstacle, but it’s important to recognize the long-term benefits of this immediate investment; reducing psychological distress from the start can lead to less problems down the road.
- Have there been efforts to publish these narratives so that other patients and health professionals can learn from these experiences?
Not so much, due to the intimacy of these narratives. Excerpts have been cited in journal articles, but these diaries have been primarily a resource for the immediate people involved in each narrative.
- How do physicians play a role in the ICU patient diaries?
It seems as though physicians are more backstage for these efforts. Nurses have adopted the ICU patient diaries as something of their own, and doctors are less involved actively in the daily care.
—
I guess that’s what I’m trying to push again with my illness narrative research. I am glad to see that health professionals such as nurses are becoming more involved in narrative work, but I think that this is just as crucial for physicians. There may not be time for this level of engagement on each person’s part, but I believe that at least an awareness by all health professionals would make a difference.
Filed under Miscellaneous Musings, Narrative Medicine Research